It’s day 2 of our week-long conversation about why the colon cancer community needs to begin the conversation about screening before 50. Thanks for tuning in! Yesterday, we learned about Karen Walsh and her powerful advocacy.
Karen was the keynote speaker at the 2016 NCCRT (National Colorectal Cancer Roundtable) and delivered an engaging, heart-wrenching picture of what it means to have Early Age Onset Colorectal Cancer (EAO-CRC). In her address, she delicately took to task the entire colon cancer community, asking big questions. We’re paraphrasing, but part of her address went something like this: “I never knew about the symptoms…, I never knew a family history was important, but once I did find out and asked my family both my parents had polyps and my grandmother has actually had CRC. I know that you can’t screen everyone who is younger than 50 but what might have been different if I had only known earlier?”
She’s right. We can’t screen everyone under 50, nor is that necessary to do so. What we can do – what we MUST do – is provide better information. We need to provide better answers to Karen’s questions because, let’s be honest, if Karen’s asking them, other people must be as well.
What are the symptoms of colon cancer? Should I ask my family about their previous colonoscopies? Did my parents or grandparents have polyps removed? Should I be screened earlier than 50?
These are huge questions, but they are lifesaving questions. For example, one of our staff members lost her father to colon cancer in 2016 and, because of her family history, went for a colonoscopy herself. At the age of 29, her gastroenterologist removed two polyps. She is glad she was screened for many reasons.
First, she prevented colon cancer for herself. Second, she now has a great deal more information about how often she should receive surveillance screenings and even when her children should begin screening. (Hint: It’s much earlier than 50.) She also took the opportunity to have genetic testing performed so that she has a more complete risk profile to consider and share with her family.
In the fight against colon cancer, knowledge is power. The more we know about our family history, symptoms, risk behaviors, and proclivity, the better we can make good decisions for our own health. For many people, having a colonoscopy at 50 is appropriate. But for many others, they need to be screened much earlier.
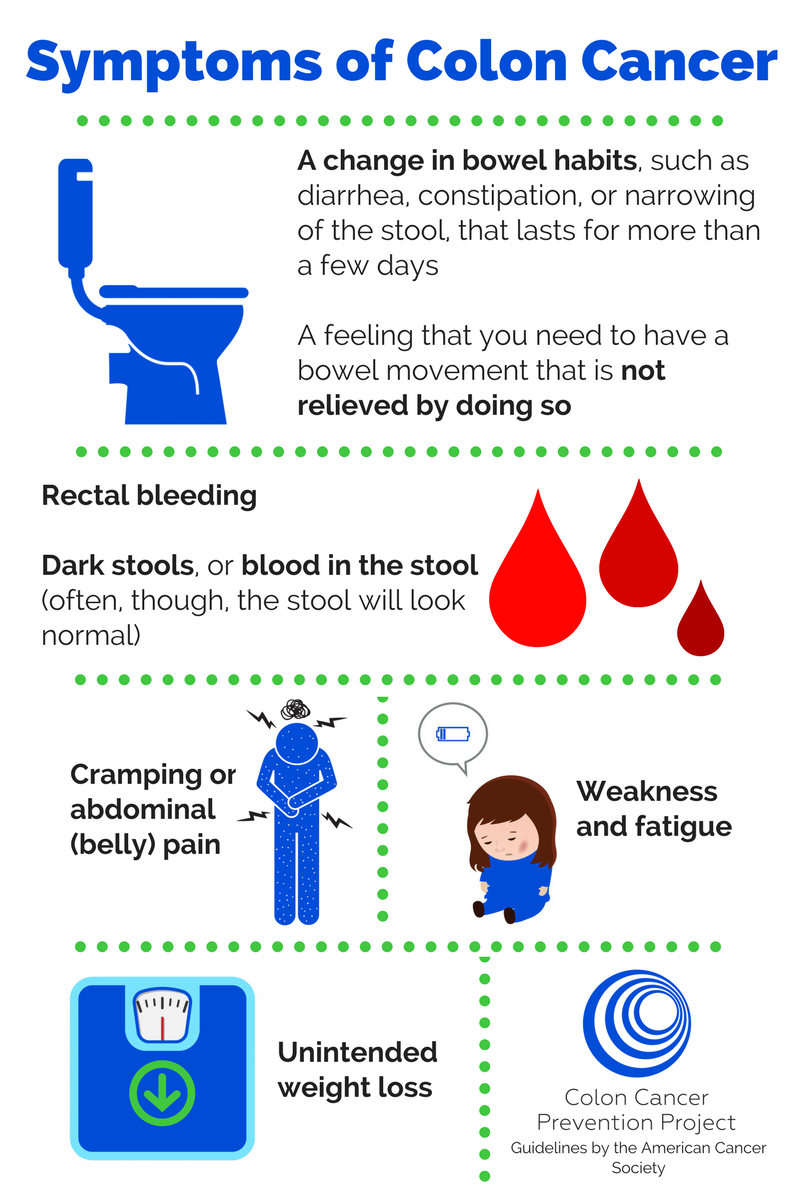
Check out these infographics and inform yourself. This first infographic highlights symptoms of colon cancer. Did you know them?
If you are experiencing any of these symptoms, talk to your doctor! We know it’s not always pleasant or comfortable to talk about your bowel movements, either in terms of frequency or consistency, but it’s important! Informing your doctor about any changes in your bowel habits, or any of the other symptoms listed, is essential to catching colon cancer at an earlier stage.
This second infographic is just as important. It emphasizes how essential it is to know your family history and risk factors. Even if you don’t need to have a colonoscopy until 50, you should be having this conversation with your doctor MUCH earlier. Having a parent with polyps will alter your appropriate screening age. Having an inflammatory bowel disease (such as Crohn’s) is another risk factor. When you know your family history and risks (such as smoking), you can have a productive conversation with your doctor about when you should be screened.
We can’t speak for the whole colon cancer community, but speaking for ourselves, we are so glad that Karen had the passion and courage to ask those questions. It shined a light on where we need to be doing more and how we can better reach people in a timely fashion. Remember – on-time screenings save lives.
We’re continuing the conversation for the rest of the week, delving into what we’re asking from the medical community in terms of policy change, what we need from you as advocates, and how, together, we can dramatically tip the scales in the favor of fewer diagnoses of colon cancer. We hope you’ll stay tuned!

You must be logged in to post a comment.